 Earth Day began in 1970 as an event to raise awareness of our environment. What began as a single day in April is now recognized around the world to bring
Read more
Earth Day began in 1970 as an event to raise awareness of our environment. What began as a single day in April is now recognized around the world to bring
Read more
-
Make Every Day Earth Day
posted: Apr. 16, 2024.
 Earth Day began in 1970 as an event to raise awareness of our environment. What began as a single day in April is now recognized around the world to bring
Read more
Earth Day began in 1970 as an event to raise awareness of our environment. What began as a single day in April is now recognized around the world to bring
Read more
-
The Importance of Oral Cancer Screenings
posted: Apr. 09, 2024.
 In our continuing efforts to provide the most advanced technology and highest quality care available to our patients at Family Dentistry of West Salem, we proudly screen our patients for
Read more
In our continuing efforts to provide the most advanced technology and highest quality care available to our patients at Family Dentistry of West Salem, we proudly screen our patients for
Read more
-
This April, Let’s Celebrate National Facial Protection Month!
posted: Apr. 02, 2024.
 Poor April. While other months celebrate romance, or giving thanks, or costumes and candy, April has—April Fool’s Day and a tax deadline. We might be forgiven for thinking these two
Read more
Poor April. While other months celebrate romance, or giving thanks, or costumes and candy, April has—April Fool’s Day and a tax deadline. We might be forgiven for thinking these two
Read more
-
Should Children Use Whitening Products?
posted: Mar. 26, 2024.
 As adults, we often wish our teeth could be as white as they were when we were small children. Baby teeth have thinner and whiter enamel than adult teeth, and
Read more
As adults, we often wish our teeth could be as white as they were when we were small children. Baby teeth have thinner and whiter enamel than adult teeth, and
Read more
-
What NOT to Eat after Wisdom Teeth Extraction
posted: Mar. 19, 2024.
 Now that you’re having your wisdom teeth removed at our WEST SALEM, Wisconsin office, you’re probably looking forward to spending a few days on the couch with a cool dish
Read more
Now that you’re having your wisdom teeth removed at our WEST SALEM, Wisconsin office, you’re probably looking forward to spending a few days on the couch with a cool dish
Read more
-
St. Patrick's Day: Celtic pride, green shamrocks, and lucky charms!
posted: Mar. 12, 2024.
 “St. Patrick's Day is an enchanted time -- a day to begin transforming winter's dreams into summer's magic.” Adrienne Cook
Lucky green shamrocks, leprechauns, and pots of gold – it must
Read more
“St. Patrick's Day is an enchanted time -- a day to begin transforming winter's dreams into summer's magic.” Adrienne Cook
Lucky green shamrocks, leprechauns, and pots of gold – it must
Read more
-
Good Nutrition Leads to Healthy Mouths
posted: Mar. 05, 2024.
 At Family Dentistry of West Salem, we know the most common oral health diseases are tooth decay and periodontal disease (or gum disease), and both are among the easiest to
Read more
At Family Dentistry of West Salem, we know the most common oral health diseases are tooth decay and periodontal disease (or gum disease), and both are among the easiest to
Read more
-
Avoid the Emergency Room for Dental Problems
posted: Feb. 27, 2024.
 There are certainly situations when going to an emergency room is the best response for your problem. A severe injury to your mouth, jaw, or face would qualify.
However, when it
Read more
There are certainly situations when going to an emergency room is the best response for your problem. A severe injury to your mouth, jaw, or face would qualify.
However, when it
Read more
-
Considerations When Picking the Right Mouthwash
posted: Feb. 20, 2024.
 A solid oral health routine begins with daily brushing, flossing, and rinsing. Without a consistent oral health regimen, you may begin to experience tooth decay and bacterial infections. Few patients
Read more
A solid oral health routine begins with daily brushing, flossing, and rinsing. Without a consistent oral health regimen, you may begin to experience tooth decay and bacterial infections. Few patients
Read more
-
The Origins of Valentine's Day
posted: Feb. 13, 2024.
 When we think of Valentine’s Day, we think of cards, flowers, and chocolates. We think of girlfriends celebrating being single together and couples celebrating their relationship. We think of all
Read more
When we think of Valentine’s Day, we think of cards, flowers, and chocolates. We think of girlfriends celebrating being single together and couples celebrating their relationship. We think of all
Read more
-
Is there a connection between oral health and school performance?
posted: Feb. 06, 2024.
 As a parent, you want the best for your children, and that includes doing their best in school. You can support them by taking an interest in their activities, being
Read more
As a parent, you want the best for your children, and that includes doing their best in school. You can support them by taking an interest in their activities, being
Read more
-
Electric or Manual Toothbrush: Why It Does (and Doesn't) Matter
posted: Jan. 30, 2024.
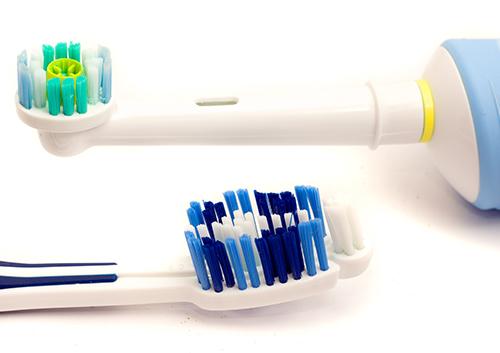 You live in the golden age of toothbrushes. Until a few decades people used twigs or brushes made from animal hair to clean their teeth: not very soft and none
Read more
You live in the golden age of toothbrushes. Until a few decades people used twigs or brushes made from animal hair to clean their teeth: not very soft and none
Read more
-
Tips for Managing Oral Pain
posted: Jan. 23, 2024.
 Experiencing tooth or oral pain is not fun. If you cannot get to Family Dentistry of West Salem right away, the pain may even seem to increase. The old saying
Read more
Experiencing tooth or oral pain is not fun. If you cannot get to Family Dentistry of West Salem right away, the pain may even seem to increase. The old saying
Read more
-
Adults Can Get Cavities Too
posted: Jan. 16, 2024.
 Sure, you brush your teeth and floss regularly, so you might think you’re off the hook when it comes to the dental chair. However, it’s just as important for adults
Read more
Sure, you brush your teeth and floss regularly, so you might think you’re off the hook when it comes to the dental chair. However, it’s just as important for adults
Read more
-
Is there really a link between my mouth and heart?
posted: Jan. 09, 2024.
 Yes, indeed! While brushing, flossing, and regular visits to Family Dentistry of West Salem are all key to maintaining a healthy smile and mouth, the doctor and our team want
Read more
Yes, indeed! While brushing, flossing, and regular visits to Family Dentistry of West Salem are all key to maintaining a healthy smile and mouth, the doctor and our team want
Read more
-
Make this the Year You Stop Smoking
posted: Jan. 02, 2024.
 It’s a new year, and it couldn’t come fast enough for many of us! Let’s do our part to make this a better year in every way—and you can start
Read more
It’s a new year, and it couldn’t come fast enough for many of us! Let’s do our part to make this a better year in every way—and you can start
Read more
Contact Us
Send Us an Email
Our Location
Find us on the map
Hours of Operation
Our Regular Schedule
Monday:
8:00 am-5:00 pm
Tuesday:
8:00 am-5:00 pm
Wednesday:
8:00 am-5:00 pm
Thursday:
7:00 am-12:00 pm
Friday:
7:00 am-3:00 pm
Saturday:
Closed
Sunday:
Closed
